TMS for Depression
TMS is FDA-approved for the treatment of major depressive disorder, including treatment-resistant depression. Depression has the strongest and most extensively studied evidence base of any condition treated with TMS, with decades of clinical research and thousands of patients studied across multiple protocols.
If you are considering TMS for depression, this page covers how it works, who is a candidate, what the research shows, and what to expect.
How TMS Works for Depression
TMS targets the left dorsolateral prefrontal cortex (DLPFC), a brain region involved in mood regulation that is consistently underactive in patients with depression. Focused magnetic pulses stimulate this area, increasing neural activity in circuits that medication may not effectively reach.
Standard Protocols
Daily sessions delivered over 4 to 6 weeks. This is the most extensively studied approach and is typically covered by insurance when treatment-resistant criteria are met.
Accelerated Protocols
Compressed treatment timelines using theta burst stimulation or multiple daily sessions, delivering the full treatment course in a shorter period.
One-Day Accelerated Protocol
The entire treatment course delivered in a single day. This is our most time-efficient and cost-effective option.
The protocol decision is made during your consultation with Dr. Nazarani based on your clinical picture, treatment history, and practical needs.
Who Is a Candidate?
You have tried medication without adequate results.
This is the most common pathway to TMS for depression. If one or more antidepressants have not provided sufficient improvement, or if side effects have made medication difficult to tolerate, TMS is a clinically supported next step. Insurance typically covers standard TMS protocols for depression when treatment-resistant criteria are met.
You prefer a non-medication approach.
Some patients want to pursue TMS before trying medication, or instead of medication entirely. This is a valid clinical choice, available as a self-pay option.
TMS for depression is not appropriate for patients with metal implants in or near the head, a history of seizures, or certain neurological conditions. Candidacy is evaluated during your consultation.
What the Research Shows
Depression has the most robust evidence base of any condition treated with TMS. The data below summarizes outcomes across standard and accelerated protocols.
Standard Protocols
In large clinical studies, approximately 50–60% of patients with treatment-resistant depression respond to a standard TMS protocol, and approximately 30–35% achieve full remission. Among those who respond, roughly 60–65% maintain their improvement at 12 months.
Accelerated Protocols
Newer accelerated protocols have demonstrated substantially higher outcomes in early research. The Stanford SAINT trial, a randomized controlled trial of 5-day accelerated TMS, reported a 79% remission rate in patients with severe treatment-resistant depression.
One-Day Accelerated Protocol
A single-day accelerated protocol (ONE-D) has reported response rates of approximately 80–90% and remission rates of 56–75% by 6 weeks, with results sustained through 12 weeks. These findings come from an initial 32-patient open-label case series. A larger propensity-matched comparison of 106 single-day patients versus 191 standard-protocol patients found approximately 50% remission with the single-day approach compared to approximately 25% with standard treatment at 6 weeks. No randomized controlled trial of single-day TMS has been completed, and larger studies are underway.
For Context
In the landmark STAR*D trial, the largest study of antidepressant medication, approximately one-third of patients achieved remission with their first medication. By the fourth medication trial, remission rates dropped below 10%.
Not everyone responds to TMS. Individual results vary, and Dr. Nazarani will discuss realistic expectations during your consultation.
Sources: Carpenter et al. (2012), Dunner et al. (2014), Cole et al. (2022), Vaughn et al. (2025), Berlow et al. (preprint), Rush et al. (2006).
What else you should know
This page covers TMS for depression specifically. For details on how TMS treatment works, what sessions feel like, and cost and insurance information, see our TMS Overview.
Frequently Asked Questions
Yes. Treatment-resistant depression is one of the primary indications for TMS. It works through a different mechanism than medication, targeting brain circuits directly rather than altering neurochemistry systemically.
In most cases, yes. Dr. Nazarani reviews your current medications during the evaluation and advises on any adjustments needed before or during treatment.
Among patients who respond to standard TMS, roughly 60–65% maintain their improvement at 12 months. Some patients benefit from periodic maintenance sessions. Durability varies by individual and protocol.
Early research suggests comparable or higher outcomes with accelerated single-day protocols, though the evidence base is newer and based on smaller studies. The One-Day Protocol is the most time-efficient and cost-effective option. Dr. Nazarani can help you determine which protocol is the best fit.
Learn More About TMS
 Depression
DepressionMehboob Ali Nazarani, M.D. · Feb 1, 2025 · 4 min read
Why Can't I Feel Happy Anymore? Causes & Treatments for Emotional Numbness
Struggling with emotional numbness or loss of joy? Learn the causes, symptoms, and treatments, including rTMS, to restore happiness and motivation.
Read article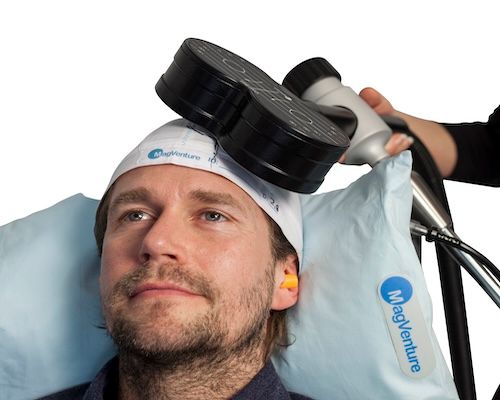 Depression
DepressionMehboob Ali Nazarani, M.D. · Dec 10, 2024 · 3 min read
Is TMS Appropriate for Me?
Learn if TMS therapy is right for you. Explore its benefits, who it helps, and what to expect, including suitability and common side effects in this comprehensive guide.
Read article Depression
DepressionMehboob Ali Nazarani, M.D. · Dec 10, 2024 · 2 min read
Long-Term Benefits of TMS Therapy - Sustaining Relief from Depression
Discover how TMS therapy offers long-lasting relief for treatment-resistant depression. Learn about its durability, low relapse rates, and effectiveness as a non-invasive, drug-free treatment.
Read articleFind Out If TMS for Depression Is Right for You
The first step is a consultation with Dr. Nazarani to evaluate whether TMS is appropriate for your situation and which protocol fits best. You are not committing to treatment — you are finding out if it makes sense for you.