TMS Therapy
TMS Therapy for Depression, OCD, and Anxiety
When medication alone is not enough, TMS offers a different path forward.
Available in Tomball | Coming soon to Houston
What Is TMS?
Transcranial Magnetic Stimulation (TMS) is a brain stimulation treatment used for depression, OCD, and anxiety. It uses focused magnetic pulses to activate specific areas of the brain involved in mood and behavior regulation, targeting neural circuits directly and reaching areas that medication alone may not effectively address.
TMS is not electroconvulsive therapy (ECT). The two are often confused, but they are fundamentally different. TMS requires no anesthesia, no sedation, and produces no memory-related side effects. You sit in a chair, remain fully awake during treatment, and return to your day immediately after.

Your TMS Doctor
Dr. Mehboob Ali Nazarani is a board-certified psychiatrist with nearly three decades of clinical experience. He founded Everhealth in 2004 and serves as its Medical Director.
Dr. Nazarani completed a Visiting Fellowship in Transcranial Magnetic Stimulation at Duke University Medical Center. He personally evaluates every TMS patient at Everhealth, performs brain mapping, selects the treatment protocol, and monitors progress throughout the treatment course.
At Everhealth, TMS is a psychiatrist-led service from start to finish. The doctor who designs your treatment plan is the same one who evaluates you, maps your brain, and adjusts your protocol based on your response.
Who Is a Candidate?
You have tried medication without the results you need
If one or more medications have not provided adequate improvement, or if side effects have made medication difficult to tolerate, TMS is a clinically supported next step. This is the most common pathway to TMS, and insurance typically covers treatment for FDA-approved conditions when medication has not been effective.
You prefer a non-medication approach
Some patients want to pursue TMS before trying medication, or instead of medication entirely. That is a valid clinical choice, and one we support. This pathway is available as a self-pay option.
Your condition is treated off-label
TMS is FDA-approved for depression and OCD. For conditions like generalized anxiety, TMS is used off-label based on a growing body of research. We discuss the current evidence during your consultation so you can make an informed decision.
Whether you are new to Everhealth or already a patient here, TMS is available to you. Existing patients can be referred internally by their provider. If you are new to the practice and specifically interested in TMS, you can request a consultation directly.
TMS is not appropriate for everyone. Patients with metal implants in or near the head, a history of seizures, or certain neurological conditions may not be candidates. This is evaluated during your consultation.
Conditions We Treat
TMS works differently depending on the condition being treated. Each involves specific brain targets, distinct protocols, and its own body of clinical evidence. Select your condition below to see how TMS applies to your situation and what the research shows.
Depression
TMS has the strongest and deepest evidence base of any condition it treats. For patients with treatment-resistant depression, it is one of the most effective non-medication options available.
Learn more about TMS for Depression →FDA-ApprovedAdolescent Depression
TMS is FDA-approved for adolescent depression, with age-appropriate protocols and growing clinical evidence in younger populations.
Learn more about TMS for Adolescent Depression →FDA-ApprovedOCD
TMS for OCD uses different brain targets and protocols than depression treatment. It is FDA-approved and supported by a growing body of clinical research, particularly for patients who have not responded adequately to therapy and medication alone.
Learn more about TMS for OCD →Off-LabelAnxiety / GAD
TMS for generalized anxiety is used off-label, with emerging clinical evidence supporting its effectiveness.
Learn more about TMS for Anxiety →Our TMS Protocols
Not every patient needs the same treatment approach. We offer multiple TMS protocols, and the right one depends on your condition, clinical picture, and practical needs. The protocol decision is made during your consultation with Dr. Nazarani.
Standard Protocols
Daily sessions delivered over 4 to 6 weeks. This is the most extensively studied TMS approach with the deepest evidence base. Standard protocols are available for depression and OCD, and are typically covered by insurance for FDA-approved conditions.
One-Day Accelerated Protocol
The entire TMS treatment course delivered in a single day. No weeks of daily visits, no extended time away from work or family. This is our most time-efficient and cost-effective TMS option, and it is available for patients traveling from outside the Greater Houston area.
Accelerated and Tailored Protocols
Compressed treatment schedules, theta burst stimulation, enhanced protocols, and other approaches customized to the patient's condition and clinical picture. These options are well-suited for patients who need a faster timeline or a more individualized approach, and are available for depression, OCD, and anxiety.
What the Process Looks Like
- 1
Consultation
The process begins with a clinical evaluation. Dr. Nazarani reviews your diagnosis, treatment history, and current symptoms to determine whether TMS is appropriate and which protocol fits best.
- 2
Brain Mapping
Before treatment begins, Dr. Nazarani performs brain mapping to identify the precise treatment target. The motor threshold is calibrated to your individual neuroanatomy, and the stimulation site is determined based on your condition and the protocol selected.
- 3
Treatment Sessions
Treatment is delivered at our Tomball office by a trained TMS technician. Session length varies by protocol. Standard sessions take approximately 19 minutes. Theta burst sessions can be completed in approximately 3 minutes. You are seated comfortably, fully awake, and can return to normal activities immediately after.
- 4
Monitoring
Your progress is tracked throughout the treatment course using standardized clinical measures. If adjustments to the protocol are needed, whether in targeting, intensity, or approach, Dr. Nazarani reviews your response data and modifies the plan accordingly.
- 5
Post-Treatment
After the treatment course is complete, we discuss your response and plan next steps. For some patients that means maintenance sessions. For others it means continuing with their existing care plan.
What to Expect
During each session, you will feel a tapping or clicking sensation on your scalp at the treatment site. Most patients find it mildly uncomfortable at first but adjust within the first few sessions. You are fully awake throughout and can relax, read, or watch something during treatment.
The most common side effects are mild scalp discomfort and headache, both typically temporary and tend to diminish over the course of treatment. There is no sedation, no recovery period, and no cognitive side effects. Most patients return to work, school, or their daily routine immediately after each session. You do not need someone to drive you.
What the Research Shows
Standard TMS for Depression
In large clinical studies, approximately 50–60% of patients with treatment-resistant depression respond to a standard TMS protocol, and approximately 30–35% achieve full remission. Among those who respond, roughly 60–65% maintain their improvement at 12 months.
Accelerated and One-Day Protocols
Newer accelerated protocols have demonstrated substantially higher outcomes in early research. The Stanford SAINT trial, a randomized controlled trial of 5-day accelerated TMS, reported a 79% remission rate in patients with severe treatment-resistant depression. A single-day accelerated protocol (ONE-D) has reported response rates of approximately 80–90% and remission rates of 56–75% by 6 weeks, with results sustained through 12 weeks. These findings come from an initial 32-patient open-label case series. No randomized controlled trial of single-day TMS has been completed, and larger studies are underway.
For Context
In the landmark STAR*D trial, the largest clinical study of antidepressant medication, approximately one-third of patients achieved remission with their first medication. By the fourth medication trial, remission rates dropped below 10%.
Condition-specific research and outcomes are detailed on each treatment page.
Sources: Carpenter et al. (2012), Dunner et al. (2014), Cole et al. (2022), Vaughn et al. (2025), Rush et al. (2006).
What Our TMS Patients Say

Finding Resilience and Renewal: Susan's TMS Success Story
After 30 years of medication stopped working, Susan regained her quality of life and social connections through non-chemical TMS therapy. The treatment proved life-changing, providing her with the emotional strength and equanimity to navigate a serious health diagnosis with hope.

Reclaiming Motivation and Life: Danielle's TMS Success Story
After struggling with depression and a lack of motivation that left her unable to leave bed, Danielle found lasting relief and renewed energy through TMS treatment. She now enjoys a vibrant social life and personal passions.
Cost and Insurance
We discuss cost before treatment begins. There are no surprise bills.
Insurance Coverage
For FDA-approved conditions (depression, adolescent depression, OCD), insurance may cover standard TMS protocols when treatment-resistant criteria are met. This typically means one or more prior medication trials that were ineffective or not tolerated. We verify your insurance coverage as part of the TMS evaluation process and let you know what to expect before treatment starts.
Self-Pay
For patients pursuing TMS as a first-line option, for off-label conditions such as anxiety, or when insurance does not cover treatment, self-pay is available. The One-Day Accelerated Protocol starts from $2,000 and is the most cost-effective TMS option we offer.
Financing and Flexibility
CareCredit is available as a financing option. We can also work with patients on pricing on a case-by-case basis to make treatment accessible.
Location and Access
TMS is available at our Tomball office, with Houston coming soon. For patients pursuing the One-Day Accelerated Protocol, our Tomball location serves patients from across Greater Houston, Texas, and beyond.
Tomball
TMS AvailableTomball, TX 77377
Frequently Asked Questions
TMS is FDA-approved and has been used in clinical practice for over 15 years. The most common side effects are mild scalp discomfort and headache, both typically temporary. Serious side effects are rare.
TMS and ECT are fundamentally different treatments. TMS is non-invasive, requires no anesthesia or sedation, and produces no memory-related side effects. You are awake during treatment and can drive yourself home afterward.
In most cases, yes. Dr. Nazarani reviews your current medications during the evaluation and advises on any adjustments needed before or during treatment.
Response time varies by individual and protocol. Some patients notice improvement within the first few weeks of a standard treatment course. For the One-Day Protocol, improvement typically develops over the weeks following treatment, with full effects emerging by approximately four to six weeks.
No referral is required. You can contact us directly to request a TMS consultation. If you are already a patient at Everhealth, your provider can refer you internally.
Yes. Some patients prefer a non-medication approach, and that is a valid clinical choice. This pathway is available as a self-pay option, and Dr. Nazarani will discuss whether TMS is appropriate for your specific situation during the consultation.
Not everyone responds to TMS. If treatment is not effective, Dr. Nazarani will discuss alternative options with you. We are straightforward about this because setting realistic expectations is part of how we approach care.
Learn More About TMS
 Depression
DepressionMehboob Ali Nazarani, M.D. · Feb 1, 2025 · 4 min read
Why Can't I Feel Happy Anymore? Causes & Treatments for Emotional Numbness
Struggling with emotional numbness or loss of joy? Learn the causes, symptoms, and treatments, including rTMS, to restore happiness and motivation.
Read article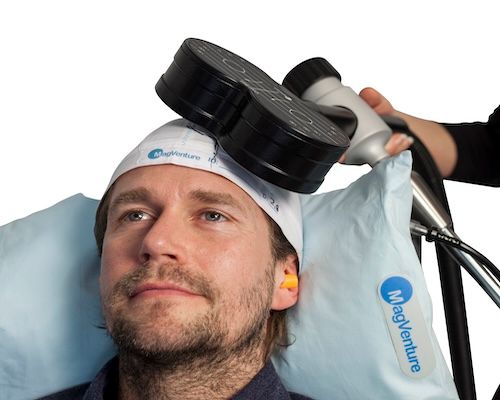 Depression
DepressionMehboob Ali Nazarani, M.D. · Dec 10, 2024 · 3 min read
Is TMS Appropriate for Me?
Learn if TMS therapy is right for you. Explore its benefits, who it helps, and what to expect, including suitability and common side effects in this comprehensive guide.
Read article Depression
DepressionMehboob Ali Nazarani, M.D. · Dec 10, 2024 · 2 min read
Long-Term Benefits of TMS Therapy - Sustaining Relief from Depression
Discover how TMS therapy offers long-lasting relief for treatment-resistant depression. Learn about its durability, low relapse rates, and effectiveness as a non-invasive, drug-free treatment.
Read articleFind Out If TMS Is Right for You
The first step is a consultation with Dr. Nazarani to evaluate whether TMS is appropriate for your situation and which protocol fits best. You are not committing to treatment. You are finding out if it makes sense for you.
